Contents
Electronic Health Records are no longer just digital filing systems. They are the backbone of modern healthcare delivery. However, many healthcare organizations still rely on legacy EHR systems that struggle with interoperability, security vulnerabilities, outdated interfaces, and performance limitations.
According to a report by Fortune Business Insights, the global EHR market was valued at USD 29.68 billion in 2023 and is projected to reach USD 46.63 billion by 2032. This growth highlights how critical EHR platforms have become in enabling connected, data-driven healthcare ecosystems.
To stay competitive and compliant, healthcare providers must modernize their EHR systems. Leveraging professional custom EHR software development services is essential in this journey, as EHR modernization is not simply about upgrading technology. It involves re-architecting systems for scalability, improving interoperability, strengthening data security, enhancing user experience, and aligning with evolving regulatory standards such as HIPAA.
In this guide, we will explore:
- The benefits of EHR modernization
- Different modernization approaches
- Step-by-step modernization process
- Common challenges and practical solutions
- Key considerations to ensure a successful transformation
Modernizing legacy EHR systems is a strategic step toward building a more connected, secure, and scalable healthcare environment. As organizations move beyond outdated infrastructure, exploring EHR software development helps in re-architecting systems for interoperability, compliance, and long-term growth. With the right strategy, modernization not only improves performance but also enables better patient outcomes and operational efficiency.
What is EHR Modernization?
EHR modernization is the process of upgrading or replacing legacy electronic health record systems with contemporary technology solutions. This transformation improves system performance, security, and interoperability while preserving valuable historical patient data.
Unlike simple software updates, EHR modernization involves fundamental changes to system architecture. Organizations migrate from outdated on-premises infrastructure to cloud-based environments. Modern APIs replace proprietary interfaces that limited integration capabilities. User experiences improve through redesigned interfaces built on current design principles.
Modernization initiatives take various forms depending on organizational needs and constraints. Some healthcare providers choose to replace their entire system with modern EHR platforms. Others prefer incremental upgrades that gradually transform legacy systems without full replacement. Hybrid approaches combine both strategies to balance risk with transformation speed.
Why Healthcare Organizations Need EHR Modernization
Legacy EHR systems create compounding challenges that affect every aspect of healthcare operations. Understanding these helps justify modernization investments to stakeholders across the organization.
1. Aging technology limits clinical efficiency
Outdated EHR platforms significantly slow down clinical workflows. Physicians spend excessive time clicking through cumbersome interfaces designed decades ago. Nurses duplicate data entry across disconnected system modules. These inefficiencies steal time from direct patient care activities.
System performance degrades as databases grow and hardware ages. Response times increase while user frustration mounts daily. Staff develop workarounds that create inconsistent processes and documentation gaps.
Modern EHR systems streamline workflows through intelligent design. Fewer clicks accomplish common tasks while automation handles routine documentation. Clinical staff reclaim time for activities that directly benefit patient outcomes.
2. Maintenance costs consume IT budgets
Supporting legacy systems requires specialized expertise that becomes increasingly scarce. Developers familiar with outdated programming languages command premium rates. Hardware maintenance for aging infrastructure adds unpredictable expenses year-round.
Vendor support contracts for older EHR versions typically cost more than current releases. Some vendors charge premium fees for extended support on discontinued products. Eventually, vendors end support entirely, leaving organizations without security patches or bug fixes.
Modernization eliminates these escalating maintenance burdens. Cloud-based systems shift infrastructure management to service providers with economies of scale. Current software versions receive regular updates included in standard subscription pricing.
3. Integration challenges isolate patient data
Legacy systems often lack modern integration capabilities. Proprietary interfaces make connecting with newer healthcare applications difficult and expensive. Patient data remains trapped in silos, preventing comprehensive care coordination.
Healthcare interoperability standards like FHIR require modern system capabilities. Legacy platforms cannot easily meet the data exchange requirements of payers and regulatory bodies. Organizations miss opportunities to participate in health information exchanges and care networks.
Modern EHR architecture embraces open standards and API-based integration. Connecting with external systems becomes straightforward rather than exceptional. Data flows freely between applications to support coordinated care delivery.
4. Security vulnerabilities create compliance risks
Aging systems often lack the security features required by current regulations. Encryption standards that met requirements years ago no longer satisfy HIPAA security rules. Access control mechanisms may not support modern authentication requirements.
Cybersecurity threats have evolved dramatically since legacy systems were designed. Attack techniques that did not exist when older platforms were built now target healthcare organizations daily. Systems without current security controls become attractive targets for data breaches.
EHR modernization incorporates contemporary security measures throughout the architecture. Modern encryption protects data at rest and during transmission. Advanced access controls support multi-factor authentication and zero-trust security models.
Concerned About Your Legacy EHR Security Risks?
Work with experienced healthcare software experts to enhance performance, security, and interoperability through strategic modernization.

Key Components of Modern EHR Architecture
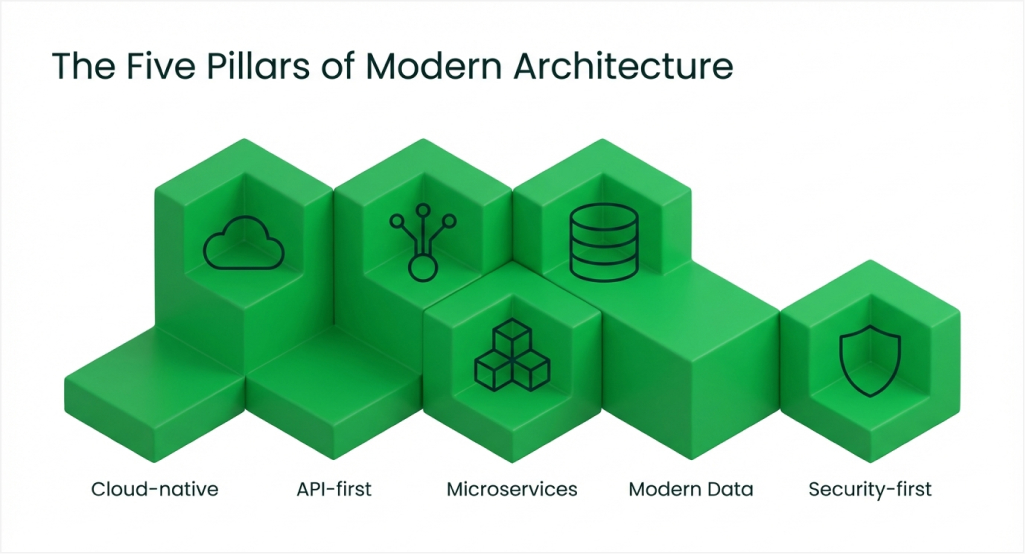
Successful modernization establishes technical foundations that support current needs while enabling future capabilities. Understanding these components helps stakeholders evaluate modernization approaches effectively.
1. Cloud-native infrastructure
Cloud architecture underpins modern EHR systems. This approach leverages managed services that reduce operational burden while improving reliability.
Essential capabilities
- Automatic scaling responds to demand fluctuations without manual intervention.
- Geographic redundancy ensures system availability during regional outages.
- Managed database services handle backup, recovery, and optimization automatically.
- Container orchestration enables efficient resource utilization and deployment flexibility.
- Infrastructure as code ensures consistent environment configurations.
- Continuous monitoring identifies performance issues before users experience impacts.
- Disaster recovery capabilities protect against data loss and extended outages.
Cloud infrastructure eliminates data center management responsibilities from healthcare IT teams. Organizations focus resources on clinical applications rather than hardware maintenance.
2. API-first integration layer
Modern systems expose functionality through well-documented application programming interfaces. This approach enables flexible integration with internal and external applications.
Essential capabilities
- RESTful APIs support standard web integration patterns.
- FHIR compliance enables healthcare-specific data exchange.
- OAuth 2.0 authentication secures API access appropriately.
- Rate limiting protects system resources from excessive requests.
- Versioning strategies maintain compatibility during API evolution.
- Developer documentation accelerates integration development.
- Sandbox environments enable safe integration testing.
API-first design transforms EHR platforms from isolated systems into extensible platforms. Third-party applications enhance functionality without compromising core system integrity.
3. Microservices architecture
Breaking monolithic applications into discrete services improves system maintainability and scalability. Each service handles specific functionality while communicating through defined interfaces.
Essential capabilities
- Independent service deployment enables targeted updates without system-wide impacts.
- Service isolation prevents failures from cascading into outages.
- Flexible technology enables optimal tools for specific service requirements.
- Horizontal scaling addresses performance needs at the service level.
- Domain-driven design aligns services with business capabilities.
- Event-driven communication enables loose coupling between services.
- Centralized logging aggregates information across distributed services.
Microservices architecture enables organizations to modernize incrementally. Individual components can be upgraded without requiring a complete system replacement.
4. Modern data management
Contemporary data architectures support both operational needs and analytical insights. Multiple data stores optimize for different access patterns and use cases.
Essential capabilities
- Operational databases handle transactional workloads with low latency.
- Data warehouses aggregate information for reporting and analysis.
- Data lakes store unstructured information for advanced analytics.
- Real-time streaming processes events as they occur.
- Master data management ensures consistency across systems.
- Data quality tools identify and remediate information issues.
- Privacy controls implement data protection requirements.
Modern data management enables artificial intelligence and machine learning applications. Historical information becomes a strategic asset rather than a storage burden.
5. Security-first design
Security is integrated throughout modern architecture rather than being added as an afterthought. Defense-in-depth strategies protect against diverse threat vectors.
Essential capabilities
- Zero-trust network architecture verifies every access request.
- End-to-end encryption protects data throughout its lifecycle.
- Identity management centralizes authentication across applications.
- Secrets management secures credentials and encryption keys.
- Security monitoring detects suspicious activities continuously.
- Automated vulnerability scanning identifies weaknesses proactively.
- Incident response automation accelerates threat containment.
Security-first design addresses compliance requirements by default. Healthcare organizations satisfy regulatory demands while protecting patient trust.
EHR Modernization Methodologies for Clinical and Operational Excellence

Organizations choose modernization strategies based on specific circumstances and objectives. Each approach offers distinct advantages and considerations.
Approach 1: Complete replacement
Full replacement involves implementing a new EHR system and retiring the legacy platform. This approach delivers comprehensive modernization but requires significant organizational change.
When to choose this approach:
- Legacy system architecture prevents incremental modernization.
- Current vendor lacks a viable upgrade path to a modern platform.
- The organization requires capabilities that are not available through upgrades.
- Total cost of ownership favors replacement over renovation.
Key considerations:
Complete replacement typically requires longer implementation timelines. Data migration complexity increases with full system changes. Staff training needs expand when interfaces and workflows change entirely. However, organizations avoid carrying technical debt forward into modernized environments.
Approach 2: Platform modernization
Platform modernization upgrades existing systems through vendor-provided migration paths. Organizations retain core EHR functionality while gaining modern infrastructure and features.
When to choose this approach:
- The current vendor offers a cloud-based, modern version of the existing product.
- Staff familiarity with existing workflows justifies continuity.
- The organization prefers managed migration with vendor support.
- Integration investments carry forward to the modernized platform.
Key considerations:
Platform modernization reduces risk through vendor-managed transition processes. Training requirements decrease when interfaces remain familiar. However, organizations remain dependent on single vendor roadmaps. The scope of modernization is limited to the capabilities the vendor provides.
Approach 3: Incremental transformation
Incremental transformation modernizes systems gradually through targeted component upgrades. Legacy elements phase out as modern replacements prove stable and effective.
When to choose this approach:
- Organizational risk tolerance requires gradual change.
- Budget constraints prevent large single-year investments.
- Critical legacy functionality lacks modern alternatives.
- Integration complexity makes rapid change impractical.
Key considerations:
Incremental approaches extend transformation timelines significantly. Organizations must maintain hybrid environments during transition periods. Integration complexity increases when legacy and modern components must coexist. However, each phase delivers value while appropriately managing risk.
Approach 4: Strangler fig pattern
This architectural pattern wraps legacy systems with modern interfaces while gradually replacing underlying functionality. External applications interact with modern facades while legacy components handle processing temporarily.
When to choose this approach:
- The legacy system serves critical functions that cannot tolerate disruption.
- Modern interface requirements exceed the capabilities of legacy systems.
- The organization wants to expose legacy data through modern APIs.
- Technical constraints prevent direct modification of the legacy system.
Key considerations:
The strangler pattern enables immediate interface modernization without legacy changes. Organizations deliver modern experiences while backend transformation continues. Complexity increases when maintaining wrapper layers alongside legacy systems. Eventually, legacy components retire completely as modern replacements mature.
The following section outlines a comprehensive framework for executing EHR modernization initiatives that ensures clinical continuity, regulatory compliance, data integrity, and scalable digital transformation.
Not Sure Which Modernization Approach Fits Your EHR System?
Our specialists help you evaluate replatforming, reengineering, and cloud migration options based on your current system architecture.
Proven EHR Modernization Framework for Scalable Healthcare Systems
Successful modernization follows a structured approachSuccessful modernization follows a structured approach that balances thorough planning with iterative execution—an approach commonly adopted by top EHR development companies to ensure consistent results. Each phase builds upon previous work to manage risk while delivering measurable value.that balances thorough planning with iterative execution. Each phase builds upon previous work to manage risk while delivering value.
Phase 1: Assessment and strategy development
Timeline: 6 to 12 weeks
Assessment establishes the foundation for all subsequent modernization activities. This phase evaluates current systems, documents requirements, and defines the modernization strategy.
Key activities:
- Current state analysis: Technical teams inventory existing systems, integrations, and data stores. Documentation gaps receive attention to ensure a complete understanding of legacy environments.
- Pain point identification: Stakeholder interviews reveal operational challenges and improvement priorities. Clinical staff provide workflow insights while IT teams describe technical limitations.
- Future state visioning: Leadership defines objectives and success criteria for modernization outcomes. Strategic goals shape technical decisions throughout subsequent phases.
- Approach selection: Technical and business factors inform modernization strategy recommendations. Cost models compare approaches to support investment decisions.
- Roadmap development: Phased implementation plans sequence work appropriately. Dependencies and milestones guide project execution.
Assessment deliverables provide reference points throughout the modernization journey. Skipping this phase leads to misaligned implementations and wasted investments.
Phase 2: Architecture design and planning
Timeline: 8 to 16 weeks
Design translates strategy into detailed technical specifications. This phase defines system architecture, integration approaches, and migration plans.
Key activities:
- Technical architecture design: Architects define infrastructure, application, and data architectures. Cloud platform selection and configuration specifications emerge from design work.
- Integration design: Detailed specifications define how modernized systems connect with retained components. API designs establish interfaces for internal and external communication.
- Security architecture: Authentication, authorization, and encryption approaches receive explicit definition. Compliance requirements shape security design decisions.
- Data migration planning: Migration scope, sequencing, and validation approaches are thoroughly planned. Data quality remediation identifies cleanup requirements before migration.
- Implementation planning: Detailed project plans define tasks, resources, and timelines. Risk mitigation strategies address identified challenges proactively.
Design review gates ensure stakeholder alignment before implementation begins. Thorough design prevents costly changes during construction phases.
Phase 3: Infrastructure and platform setup
Timeline: 4 to 8 weeks
Platform setup establishes the technical foundation for modernization activities. Cloud environments, security controls, and development tooling prepare for application work.
Key activities:
- Cloud environment provisioning: Infrastructure teams configure cloud platforms in accordance with design specifications. Network configurations, security groups, and access controls receive implementation.
- Development environment setup: Teams establish environments for development, testing, and staging. Environmental parity with production prevents deployment surprises.
- Security control implementation: Identity management, encryption, and monitoring capabilities are deployed to the platform. Security baseline is validated before application deployment begins.
- DevOps pipeline creation: Continuous integration and deployment automation accelerate subsequent development. Automated testing frameworks ensure code quality throughout the project.
Platform readiness verification confirms environments meet requirements before application work begins. Rushing platform setup creates problems that compound throughout implementation.
Phase 4: Application modernization and development
Timeline: 16 to 52 weeks, depending onthe scope
Application work transforms legacy functionality into modern implementations. Iterative development delivers value incrementally while managing technical risk.
Key activities:
- Module prioritization: Teams sequence modernization based on business value and technical dependencies. Quick wins build momentum while complex components receive appropriate attention.
- Iterative development: Sprint-based work delivers testable functionality at regular intervals. Stakeholder demonstrations gather feedback for continuous refinement.
- Integration implementation: Connections with retained systems and external applications receive development. Testing validates data flows across system boundaries.
- Quality assurance: Automated and manual testing validates functionality throughout development. Performance testing confirms systems meet capacity requirements.
Regular stakeholder engagement ensures modernization aligns with evolving organizational needs. Course corrections happen early when feedback cycles remain short.
Phase 5: Data migration and validation
Timeline: 8 to 20 weeks overlapping with application development
Data migration transfers historical information from legacy systems to modern platforms. Thorough validation ensures data integrity throughout the transition.
Key activities:
- Data profiling: Analysis reveals data quality issues requiring remediation. Volume assessments inform migration approach and resource requirements.
- Transformation development: Scripts convert legacy data formats to modern structures. Business rules handle special cases and data cleansing requirements.
- Migration testing: Multiple test cycles validate the completeness and accuracy of the migration. Performance testing ensures migration completes within acceptable windows.
- Validation and reconciliation: Systematic comparisons confirm migrated data matches source systems. Business users verify that critical information appears correctly.
- Cutover execution: Final migration transfers production data to modern systems. Rollback procedures provide safety nets against unexpected issues.
Data migration failures undermine modernization success regardless of application quality. Investment in thorough migration planning and testing pays significant dividends.
Phase 6: Training and change management
Timeline: 4 to 12 weeks overlapping with later phases
Organizational readiness determines whether technical modernization translates to operational success. Training and change management prepare staff for new systems and workflows.
Key activities:
- Training development: Role-based curricula address the needs of different user groups. Materials include documentation, videos, and hands-on exercises.
- Change communication: Regular updates inform stakeholders about the progress of modernization. Leadership messaging reinforces organizational commitment to transformation.
- Champion development: Super users receive advanced training to support peers. Champions provide first-line assistance during transition periods.
- Training delivery: Sessions prepare users before they need new system access. Practice environments enable hands-on learning without production risk.
Inadequate training investment produces user frustration and adoption resistance. Change management deserves equal attention alongside technical implementation.
Phase 7: Deployment and stabilization
Timeline: 4 to 8 weeks
Deployment transitions modernized systems to production use. Intensive support ensures stable operations while users adapt to new capabilities.
Key activities:
- Deployment execution: Cutover plans guide the systematic production transition. Monitoring confirms system health throughout deployment activities.
- Hypercare support: Intensive support resources address issues rapidly during initial operations. Quick response maintains user confidence in new systems.
- Performance tuning: Production usage reveals optimization opportunities. Adjustments ensure systems meet performance expectations under real workloads.
- Issue resolution: Problems receive prioritized attention based on impact. Root cause analysis prevents the recurrence of significant issues.
Stabilization continues until operations reach a steady state. Premature support reduction undermines the value of modernization investments.
Phase 8: Optimization and continuous improvement
Timeline: Ongoing
Post-deployment optimization maximizes value from modernization investments. Continuous improvement processes identify and implement enhancements over time.
Key activities:
- Usage analysis: Analytics reveal adoption patterns and optimization opportunities. Underutilized features receive attention through additional training or refinement.
- Enhancement implementation: Prioritized improvements are deployed through regular release cycles. User feedback shapes enhancement priorities.
- Performance monitoring: Ongoing measurement identifies degradation before users experience impacts. Proactive intervention maintains service quality.
- Technology updates: Platform updates deliver new capabilities and security improvements. Regular refresh cycles prevent technical debt accumulation.
Modernization represents a journey rather than a destination. Organizations that invest in continuous improvement sustain competitive advantages over time.
Comprehensive EHR Modernization Cost Structure and Budget Planning Model
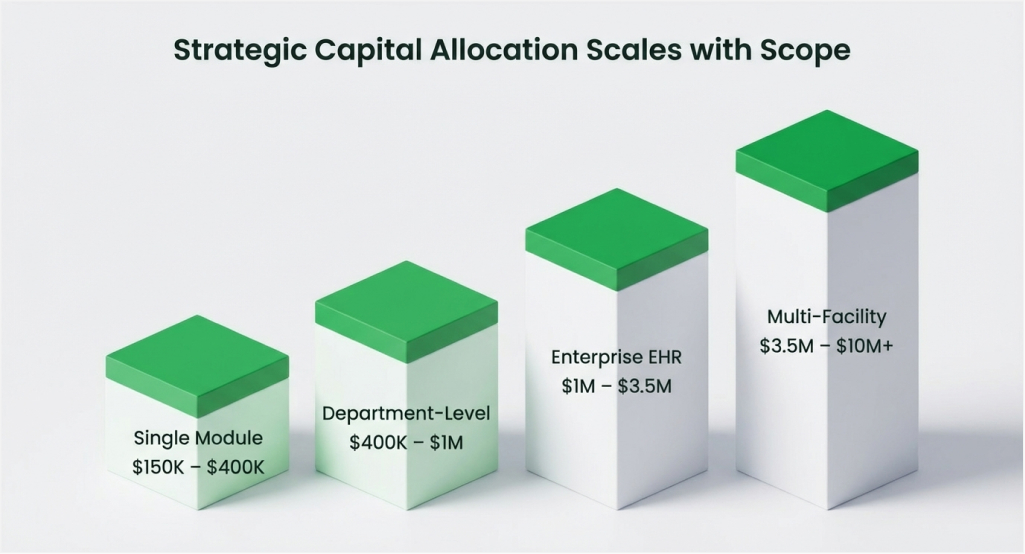
Understanding the cost components of EHR development and modernization enables accurate budgeting. Expenses vary significantly based on scope, approach, and organizational complexity.
Cost of modernization scope
| Modernization Type | Cost Range | Timeline |
|---|---|---|
| Single Module Modernization | $150,000 – $400,000 | 4-8 months |
| Department-Level Transformation | $400,000 – $1,000,000 | 8-14 months |
| Enterprise EHR Modernization | $1,000,000 – $3,500,000 | 12-24 months |
| Multi-Facility System Transformation | $3,500,000 – $10,000,000+ | 18-36 months |
Cost breakdown by project phase
| Phase | Percentage of Total Cost |
|---|---|
| Assessment & Strategy | 8-12% |
| Architecture & Design | 12-18% |
| Infrastructure Setup | 8-12% |
| Application Development | 35-45% |
| Data Migration | 10-15% |
| Training & Change Management | 8-12% |
| Deployment & Stabilization | 5-8% |
Factors that increase modernization costs
Several variables influence total investment requirements for modernization.
- Legacy system complexity: Systems with extensive customizations require more analysis and migration work. Poorly documented systems increase discovery effort and risk. Proprietary interfaces complicate integration modernization significantly.
- Data migration scope: Larger historical data volumes extend migration timelines and costs. Data quality issues requiring remediation add unplanned expenses. Complex data transformations demand specialized development effort.
- Integration requirements: Numerous external system connections multiply the cost of integration development. Legacy integration approaches require complete replacement with modern alternatives. Real-time integration needs add complexity beyond batch processing.
- Compliance requirements: Strict regulatory environments increase validation and documentation needs. Healthcare-specific certifications require additional testing and audit activities. Security requirements beyond baseline standards add implementation scope.
- Organizational readiness: Extensive training needs increase change management investments. Resistance to change extends timelines and requires additional engagement. Multiple stakeholder groups multiply communication and coordination requirements.
Ongoing cost considerations
Modernization represents an initial investment rather than the total ownership cost. Plan for ongoing expenses throughout the modernized system lifecycle.
- Cloud infrastructure: Monthly hosting costs range from $5,000 to $50,000, depending on scale and services consumed. Usage-based pricing creates variability requiring budget flexibility.
- Annual maintenance: Budget 12% to 18% of the initial modernization cost for ongoing support. Maintenance covers bug fixes, security patches, and minor enhancements.
- Continued optimization: Enhancement development typically requires $100,000 to $500,000 annually. Feature additions and performance improvements maintain system value over time.
- Compliance maintenance: Security assessments and compliance audits cost $25,000 to $75,000 annually. Changes in regulatory requirements may trigger additional modernization scope.
Get an Accurate EHR Modernization Estimate
Share your requirements with our technical team for a detailed assessment tailored to your specific environment and objectives.
Common Challenges in EHR Modernization
Even well-planned modernization projects encounter obstacles during execution. Organizations that hire EHR software developers with specialized expertise are better positioned to anticipate these challenges and enable proactive mitigation rather than reactive crisis management.
Challenge 1: Data migration complexity
Legacy systems often contain decades of patient information in proprietary formats. Data quality issues compound migration difficulty. Incomplete documentation makes understanding data structures challenging.
How to overcome this challenge
- Invest in thorough data profiling during assessment phases.
- Develop comprehensive transformation rules with input from clinical stakeholders.
- Execute multiple migration test cycles before production cutover.
- Establish clear validation criteria and reconciliation procedures.
- Maintain rollback capabilities until validation completes successfully.
Challenge 2: Integration with retained systems
Modernization rarely replaces every system simultaneously. Legacy components that remain operational must integrate with modernized platforms. Interface incompatibilities create technical obstacles.
How to overcome this challenge
- Map all integration points comprehensively during discovery.
- Design integration layers that accommodate legacy protocols.
- Build adapters that translate between old and new interface standards.
- Plan integration testing that validates end-to-end data flows.
- Thoroughly document integration specifications for ongoing maintenance.
Challenge 3: Organizational resistance to change
Staff comfortable with familiar systems resist learning new approaches. Workflow changes can be frustrating when users feel unprepared. Productivity dips during transition periods affect morale.
How to overcome this challenge
- Involve end users throughout modernization to build ownership.
- Communicate benefits clearly and consistently throughout the project.
- Provide comprehensive training tailored to different roles and skill levels.
- Identify and support champions who advocate for modernized systems.
- Address concerns promptly to prevent negative sentiment from spreading.
Challenge 4: Maintaining operations during transition
Healthcare organizations cannot pause patient care during modernization. Production systems must remain operational while transformation proceeds. Parallel operations create complexity and resource demands.
How to overcome this challenge
- Plan transition approaches that minimize impact on the production system.
- Schedule intensive migration activities during lower-volume periods.
- Build robust rollback procedures for every deployment activity.
- Staff appropriately to support both legacy and modern systems simultaneously.
- Establish clear escalation paths for production issues during transition.
Challenge 5: Scope expansion and timeline pressure
Requirements evolve as stakeholders interact with modernizing systems. Feature requests accumulate beyond initial scope definitions. Timeline pressure creates the temptation to cut quality corners.
How to overcome this challenge
- Establish formal change request processes that assess impact before approval.
- Build contingency buffers of 15% to 25% for approved additions.
- Use phased delivery to defer non-critical features to subsequent releases.
- Maintain clear prioritization criteria tied to business value.
- Protect testing and quality assurance activities from being compressed by the timeline.
Challenge 6: Knowledge transfer and documentation gaps
Legacy system expertise often resides with a few individuals. Personnel changes during modernization create knowledge risks. Inadequate documentation complicates understanding and decision-making.
How to overcome this challenge
- Capture legacy system knowledge systematically during assessment phases.
- Engage experienced staff directly in modernization planning and execution.
- Document decisions and implementations thoroughly throughout the project.
- Build knowledge redundancy to reduce dependence on specific individuals.
- Plan knowledge transfer activities as explicit project deliverables.
Best Practices for Successful EHR Modernization
Following proven practices significantly increases modernization success rates. These guidelines represent accumulated wisdom from successful healthcare technology transformations.
1. Start with a comprehensive assessment
Invest adequate time in understanding current systems before planning modernization approaches. Rushing assessment creates knowledge gaps that surface as expensive changes during implementation.
Evaluate every legacy component, integration, and data store systematically. Document dependencies that might not be obvious from system inventories alone. Interview stakeholders at every level to understand operational impacts.
Assessment findings should not surprise anyone during later phases. Thorough discovery prevents “unknown unknowns” from derailing modernization progress.
2. Define clear success criteria
Establish measurable objectives before modernization begins. Specific targets enable progress tracking and demonstrate value to stakeholders. Vague goals make success impossible to evaluate.
Balance technical metrics with operational outcomes. System performance improvements matter alongside workflow efficiency gains. User satisfaction measures capture experience changes that technical metrics miss.
Revisit success criteria throughout the project as understanding evolves. Adjust targets when circumstances change rather than chasing outdated objectives.
3. Plan for data quality investment
Data migration success depends on underlying data quality. Legacy systems often contain inconsistent, duplicate, or outdated information. Modernization presents opportunities to address quality issues systematically.
Profile data early to understand the remediation scope. Budget time and resources for cleansing activities before migration. Establish data quality standards that modernized systems will maintain.
Quality improvements deliver ongoing value beyond migration itself. Clean data enables analytics and insights that poor data prevents.
4. Prioritize security throughout modernization
Security considerations should shape every modernization decision. Retrofit security proves more expensive and less effective than building protection from the foundations.
Engage security expertise from project initiation through deployment. Architecture reviews should include security specialists who identify vulnerabilities early. Penetration testing validates security controls before production deployment.
Compliance requirements represent minimum standards rather than sufficient protection. Organizations should exceed regulatory baselines when protecting sensitive patient information.
5. Embrace iterative delivery approaches
Delivering modernization incrementally reduces risk while accelerating value realization. Stakeholders see progress and provide feedback before significant investment accumulates.
Two- to four-week iterations work well for most modernization projects. Shorter cycles create overhead that reduces team productivity. Longer intervals delay feedback and increase the cost of course correction.
Prioritize high-value capabilities early in delivery sequences. Users begin benefiting from modernization while additional features are completed. Early success builds organizational support for continued investment.
6. Invest heavily in change management
Technical modernization succeeds only when organizations adopt new capabilities. Staff resistance and inadequate preparation undermine even excellent technical implementations.
Communicate continuously throughout the modernization journey. Stakeholders need to understand why changes happen and what benefits they will receive. Silence breeds uncertainty and resistance.
Train users thoroughly before expecting them to use new systems. Rushing training or cutting preparation activities creates frustrated users and adoption failures.
7. Plan for ongoing optimization
Modernization completion marks a beginning rather than an ending. Systems require continuous improvement to maintain value over time.
Budget for enhancement development from project inception. Organizations that stop investing after deployment watch modernized systems age into new legacy problems. Continuous improvement maintains competitive advantages.
Establish feedback mechanisms that capture user suggestions and pain points. Regular enhancement releases demonstrate organizational commitment to system quality.
Modernize Your EHR System with Space-O Technologies
EHR modernization requires careful planning, structured migration, and deep healthcare domain expertise. Data integrity, regulatory compliance, integration continuity, and minimal downtime must be prioritized throughout the process. Without the right partner, modernization efforts can lead to operational disruption and cost overruns.
Partnering with Space-O Technologies enables healthcare organizations to transform legacy EHR systems into modern, high-performance platforms, including seamless EHR integration services across evolving healthcare ecosystems. Our specialized teams understand the unique challenges of healthcare technology modernization and bring proven methodologies to every engagement.
We go beyond technical implementation to address organizational readiness and change management requirements. This comprehensive approach ensures modernization investments translate to operational improvements. Security and compliance expertise protects patient data while meeting regulatory requirements throughout transformation journeys.
Our experienced architects evaluate legacy environments and recommend modernization strategies aligned with organizational objectives. Transparent assessment processes build confidence in recommended approaches. Detailed cost estimates enable accurate budgeting without unexpected surprises.
Connect with our technical consultants to discuss your EHR modernization requirements. We provide thorough assessments, realistic timelines, and customized roadmaps to help transform your legacy systems into modern healthcare technology platforms.
Frequently Asked Questions on EHR Modernization
1. What is EHR modernization?
EHR modernization is the process of upgrading or replacing legacy electronic health record systems with contemporary technology solutions. This transformation improves system performance, security, interoperability, and user experience. Modernization approaches range from complete system replacement to incremental component upgrades. The goal is to create agile, secure platforms that support current healthcare delivery needs while enabling future capabilities.
2. How much does EHR modernization cost?
EHR modernization costs range from $150,000 for single module upgrades to $10,000,000 or more for multi-facility enterprise transformations. Single module modernization typically costs $150,000 to $400,000. Department-level projects range from $400,000 to $1,000,000. Enterprise modernization costs $1,000,000 to $3,500,000. Costs depend on the complexity of the legacy system, the scope of data migration, integration requirements, and organizational size.
3. How long does EHR modernization take?
EHR modernization timelines vary from 4 months for focused module upgrades to 36 months for complex multi-facility transformations. Single-module projects typically take 4 to 8 months to complete. Department-level modernization requires 8 to 14 months. Enterprise initiatives take 12 to 24 months. Multi-facility transformations may extend to 36 months, including phased deployments across locations.
4. What are the signs that EHR modernization is needed?
Signs indicating modernization needs include slow system performance, frustrated clinical staff, and degraded user interfaces. Increasing maintenance costs for aging infrastructure signal the timing of replacement. Integration difficulties with newer healthcare applications reveal architectural limitations. Vendor announcements ending support for legacy versions create urgency. Security vulnerabilities that current controls cannot address demand modernization attention.
5. What is the difference between an EHR upgrade and modernization?
EHR upgrades install newer versions of existing software within current architectures. Modernization transforms the fundamental architecture and infrastructure of systems. Upgrades maintain existing technology approaches while adding features. Modernization involves adopting contemporary architectures such as cloud infrastructure, microservices, and API-based integration. Modernization delivers more comprehensive improvements but requires greater investment and organizational change.
6. How do we maintain compliance during EHR modernization?
Compliance maintenance during modernization requires explicit planning and ongoing attention. Engage compliance expertise from project initiation to shape requirements. Design security controls that meet current regulatory standards. Validate compliance through testing and documentation. Plan parallel operations carefully to maintain audit readiness. Document all changes thoroughly to support regulatory inquiries during transition periods.
7. What risks are associated with EHR modernization?
Key modernization risks include data migration failures that result in the corruption or loss of patient information. Integration issues may disrupt workflows spanning multiple systems. User adoption resistance can undermine operational benefits. Timeline and budget overruns strain organizational resources. Compliance gaps during transition create regulatory exposure. Experienced modernization partners help mitigate these risks through proven methodologies.
8. Can legacy EHR data be migrated to modern systems?
Yes, legacy data migrates to modern systems through carefully planned transformation processes. Migration involves extracting data from legacy systems, transforming data into modern formats, and loading it into new platforms. Data quality issues require remediation before or during migration. Validation confirms migrated information matches the source systems accurately. Historical data preservation enables continuity of care and regulatory compliance.
9. What is cloud-based EHR modernization?
Cloud-based EHR modernization moves systems from on-premises infrastructure to cloud platforms. This approach leverages managed services that reduce operational burden. Cloud infrastructure provides automatic scaling, geographic redundancy, and reduced maintenance requirements. Organizations eliminate data center management responsibilities. Monthly operational expenses replace large capital investments in hardware and facilities.
10. How do you we EHR modernization success?
EHR modernization success measurement combines technical metrics with operational outcomes. System performance improvements include response times and availability statistics. Clinical efficiency gains are measured by documenting time and workflow completion rates. User satisfaction surveys capture experience quality. Operational metrics track support ticket volumes and error rates. Financial measures evaluate cost savings and return on investment over time.



