Contents
Healthcare organizations face mounting pressure to adopt electronic health record systems. Yet, budget uncertainty remains the biggest obstacle for many decision-makers. Founders struggle to secure funding without accurate cost projections. IT directors find it challenging to justify budget requests to hospital boards.
The cost to develop an EHR system varies dramatically based on multiple factors. Simple solutions may start around $50,000, while enterprise platforms exceed $1 million. Without clear benchmarks, comparing vendor quotes becomes nearly impossible, and budget overruns can derail even the most promising projects.
Understanding EHR software development pricing helps organizations make informed investment decisions.
This guide breaks down every aspect of EHR development cost. An experienced EHR software development company, we have shared insights on the pricing factors, development phases, and ongoing expenses for building EHR systems. Explore strategies for optimizing your investment while building a compliant and scalable solution.
Factors Affecting EHR Development Cost

Multiple variables determine your final EHR software development pricing. Understanding these factors helps you anticipate expenses and make informed decisions about project scope.
1. Feature complexity and scope
The number and sophistication of features directly impact development investment. Basic patient record management costs less than comprehensive clinical decision support systems. Each additional capability increases design, development, and testing requirements.
Core features like patient demographics and appointment scheduling form the baseline. Advanced capabilities such as AI diagnostics or predictive analytics add significant complexity. Organizations must prioritize features based on genuine clinical needs rather than wish lists.
Feature scope decisions should balance immediate requirements with future scalability. Building a foundation that supports future enhancements costs more initially. However, this approach prevents the need for expensive rebuilding as needs evolve.
2. Compliance and security requirements
Healthcare software must meet rigorous regulatory standards, which add to development complexity. HIPAA compliance in the United States requires specific security controls and audit capabilities. International markets impose additional requirements, like GDPR for European operations.
Security implementations add 15% to 30% to baseline development costs. End-to-end encryption, access controls, and audit logging require specialized expertise. Penetration testing and security audits significantly extend project timelines.
Compliance certification processes represent additional expenses. ONC certification for EHR systems involves extensive documentation and testing. Organizations targeting Medicare reimbursement must meet Meaningful Use criteria.
3. Integration requirements
Connecting EHR systems to existing healthcare infrastructure creates substantial development work. Each integration point with external systems adds $15,000 to $60,000 or more. Legacy systems without modern APIs require custom middleware development.
Common integrations include laboratory information systems and pharmacy management platforms. Billing systems, imaging archives, and practice management software also need connections. Healthcare interoperability standards like HL7 FHIR significantly simplify some integrations.
Integration complexity depends heavily on the target system’s architecture. Modern cloud-based platforms with well-documented APIs integrate more easily. Older systems may require extensive reverse engineering and the development of custom adapters.
4. User interface and experience design
Quality user interface design significantly impacts clinician adoption and satisfaction. Healthcare professionals need intuitive workflows that minimize clicks during patient encounters. Poor UX design leads to workarounds that create compliance and data quality issues.
Comprehensive UX research and design add weeks to project timelines. User interviews, workflow analysis, and usability testing require dedicated expertise. Multiple design iterations based on feedback improve final outcomes considerably.
Mobile-responsive design increases development scope substantially. Native iOS and Android applications multiply the effort required for interface development. Progressive web applications offer a middle ground between cost and mobile functionality.
5. Development team location and composition
The geographic location of your development team dramatically affects hourly rates. North American developers typically charge $150 to $250 per hour. Eastern European teams range from $50 to $100 per hour, while South Asian developers cost $25 to $60 per hour.
Team composition also significantly influences total costs. Senior architects and healthcare domain experts command premium rates. Junior developers cost less but require more oversight and produce work more slowly.
Hybrid engagement models optimize both quality and cost. Onshore project managers and architects provide oversight and communication. Offshore development teams efficiently execute implementation under their guidance.
6. Project timeline and urgency
Accelerated timelines increase costs through overtime and parallel workstreams. Compressed schedules require larger teams working simultaneously on different components. Rush projects also increase error rates that require expensive remediation.
Standard development timelines allow efficient resource utilization. Teams can complete phases sequentially without costly overlap. This approach minimizes waste and produces higher quality outcomes.
Extremely tight deadlines may require compromises in scope or quality. Organizations facing urgent needs should consider EHR MVP development approaches. Launching with core features first significantly reduces timeline pressure.
7. Ongoing maintenance and support needs
Long-term support requirements should factor into total cost of ownership calculations. Annual maintenance typically costs 15% to 20% of the initial development investment. This covers bug fixes, security patches, and minor enhancements.
Support service levels directly affect ongoing expenses. 24hr support availability costs more than business hours coverage. Organizations with international operations need round-the-clock support options.
Technology choices significantly impact long-term maintenance costs. Modern frameworks with active communities reduce maintenance complexity. Custom solutions built on obscure technologies create expensive dependency risks.
Build Your EHR with Clarity, Cost Control, and Compliance
Our experts deliver a tailored EHR cost analysis aligned with your clinical workflows, security needs, and regulatory obligations.

EHR Development Cost Breakdown by System Type
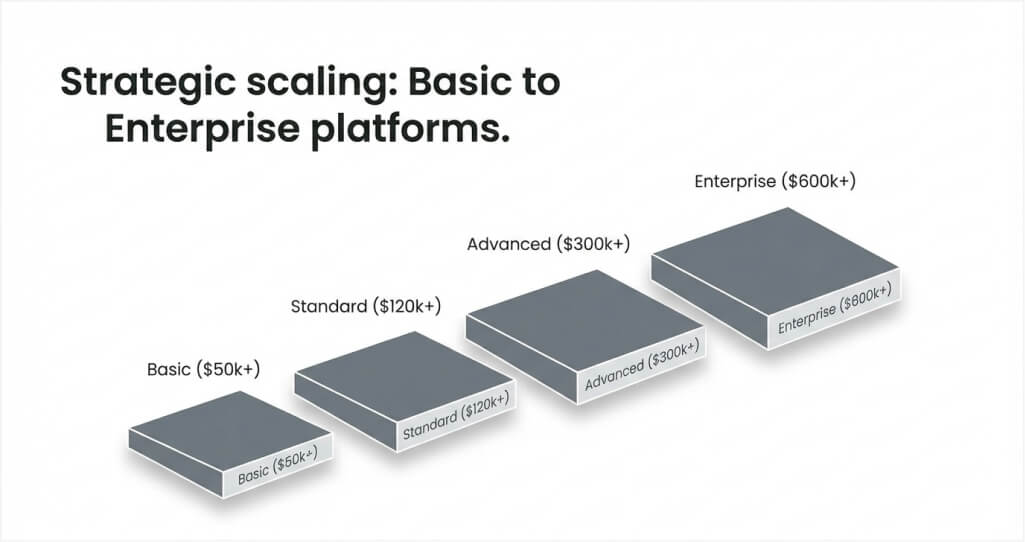
Different EHR system categories have distinct pricing ranges based on their scope and complexity. This section provides realistic cost benchmarks for various implementation types.
1. Basic EHR system
Basic EHR systems provide essential capabilities for patient record management. These solutions suit small practices or specialty clinics with straightforward workflows, including those pursuing pediatric EHR development. Development typically requires three to five months of focused effort.
Cost range: $50,000 to $120,000
Typical features include:
- Patient demographics and contact information management.
- Basic appointment scheduling and calendar functions.
- Simple clinical documentation templates.
- Prescription writing and medication lists.
- Basic reporting and data export capabilities.
- Single location deployment architecture.
- Essential security and access controls.
Basic systems work well for organizations starting their digital transformation journey. They provide a foundation that can expand as needs evolve over time.
2. Standard EHR system
Standard EHR systems offer comprehensive functionality for mid-sized healthcare organizations. These platforms support multiple providers, departments, and integrated workflows. Development timelines typically range from five to nine months.
Cost range: $120,000 to $300,000
Typical features include:
- Complete clinical documentation with specialty templates.
- Integrated billing and claims management.
- Laboratory and diagnostic result integration.
- E-prescribing with pharmacy network connectivity.
- Patient portal with secure messaging.
- Multi-provider scheduling and resource management.
- Advanced reporting and analytics dashboards.
- Mobile access for providers and patients.
Standard systems balance functionality with reasonable investment levels. They serve most ambulatory care settings and smaller hospital departments effectively.
3. Advanced EHR system
Advanced EHR systems incorporate sophisticated capabilities beyond core clinical functions. These platforms leverage artificial intelligence, predictive analytics, and comprehensive interoperability. Development requires nine to fourteen months for thorough implementation.
Cost range: $300,000 to $600,000
Typical features include:
- Clinical decision support with evidence-based recommendations.
- AI-powered documentation assistance and coding suggestions.
- Population health management and risk stratification.
- Comprehensive interoperability with external health systems.
- Telehealth integration with virtual visit capabilities.
- Advanced workflow automation and process optimization.
- Custom analytics with predictive modeling.
- Native mobile applications for iOS and Android.
Advanced systems suit organizations seeking competitive differentiation through technology. They require substantial investment but deliver significant operational improvements.
4. Enterprise EHR system
Enterprise EHR systems support large health systems with complex multi-facility operations. These platforms manage thousands of concurrent users across diverse care settings. Development takes 12 to 20 months for complete deployment.
Cost range: $600,000 to $1,500,000+
Typical features include:
- Multi-facility deployment with centralized administration.
- Comprehensive specialty module coverage.
- Advanced security with role-based access hierarchies.
- Full regulatory compliance certification support.
- Enterprise master patient index and identity management.
- Complex integration with dozens of external systems.
- Business intelligence and executive reporting platforms.
- Disaster recovery and high availability architecture.
- Dedicated training and change management tools.
Enterprise implementations represent major organizational investments. They deliver substantial returns through operational efficiency and improved care coordination.
Custom EHR Development Cost Breakdown by Phase
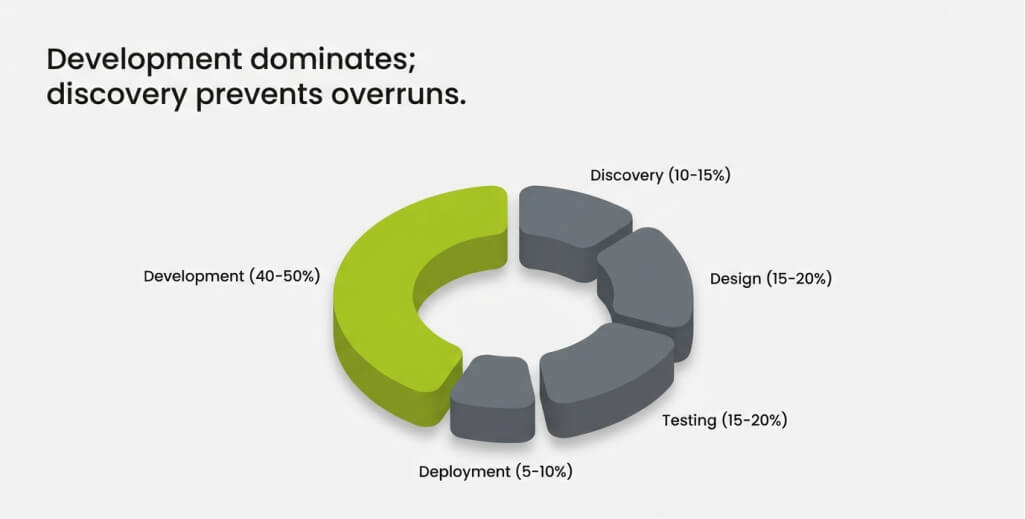
Understanding how costs distribute across development phases helps organizations plan budgets effectively when they build an EHR system. Each phase requires different expertise and delivers distinct value.
| Phase | Percentage of Total Cost | Typical Duration |
|---|---|---|
| Discovery and Requirements | 10% to 15% | 4 to 8 weeks |
| Design and Architecture | 15% to 20% | 4 to 8 weeks |
| Development and Implementation | 40% to 50% | 12 to 40 weeks |
| Testing and Quality Assurance | 15% to 20% | 6 to 12 weeks |
| Deployment and Training | 5% to 10% | 3 to 6 weeks |
Phase 1: Discovery and requirements
Discovery establishes project foundations through stakeholder interviews and workflow analysis. This phase documents current processes and identifies opportunities for improvement. Teams thoroughly assess technical environments and integration requirements.
Cost range: $10,000 to $75,000, depending on organizational complexity
Discovery investments prevent expensive scope changes during later phases. Thorough requirements documentation clearly aligns stakeholder expectations. Skipping or rushing discovery creates risks that multiply throughout development.
Phase 2: Design and architecture
Design transforms requirements into visual interfaces and technical specifications. UX designers create wireframes and interactive prototypes for validation. Technical architects define database structures and integration approaches.
Cost range: $15,000 to $100,000, depending on system complexity
Quality design reduces development rework significantly. User testing validates interfaces before expensive coding begins. Architecture decisions made here affect system performance for years to come.
Phase 3: Development and implementation
Development converts designs into functioning software through iterative coding cycles. Agile methodologies typically deliver testable features every two weeks. Product owners review progress and adjust priorities based on feedback.
Cost range: $40,000 to $600,000+, depending on scope
Development represents the largest cost component in most projects. Sprint-based delivery provides visibility into progress and burn rate. Regular demonstrations keep stakeholders engaged throughout implementation.
Phase 4: Testing and quality assurance
Testing verifies that software meets requirements and performs reliably. Functional testing validates every feature against specifications. Security testing identifies vulnerabilities before production deployment.
Cost range: $15,000 to $150,000, depending on compliance requirements
Testing investments prevent costly post launch defects and compliance issues. Automated testing enables frequent validation throughout development. Security audits and penetration testing satisfy regulatory requirements.
Phase 5: Deployment and training
Deployment transitions software from development to production environments. Carefully executed data migration moves historical information from legacy systems. Training prepares users to adopt new workflows confidently.
Cost range: $5,000 to $75,000, depending on user population
Deployment planning minimizes operational disruption during transitions. Phased rollouts effectively reduce risk in large implementations. Training investments directly impact adoption rates and return on investment.
Development Team Cost Comparison
Geographic and engagement model choices significantly impact EHR software development pricing. Understanding these options helps optimize investment without sacrificing quality.
| Region | Hourly Rate Range | Considerations |
|---|---|---|
| North America | $150 to $250 | Timezone alignment, cultural fit, and premium pricing |
| Western Europe | $100 to $180 | Strong technical education and GDPR expertise |
| Eastern Europe | $50 to $100 | Excellent value and growing healthcare expertise |
| South Asia | $25 to $60 | Cost-effective, large talent pool, and communication considerations |
| Latin America | $40 to $80 | Nearshore option, timezone overlap with North America |
Engagement model comparison
- In-house development teams provide maximum control but require significant investment. Recruiting healthcare developers takes months in competitive markets. Salary, benefits, and overhead increase effective costs substantially.
- Staff augmentation adds external developers to your existing team structure. This approach fills specific skill gaps without long-term commitments. Organizations retain technical direction while accessing specialized expertise.
- Dedicated development teams provide complete squads under vendor management. This model suits organizations without internal technical leadership. Monthly retainer pricing provides predictable costs and resource availability.
- Project-based engagement defines scope and deliverables through fixed-price contracts. This approach effectively transfers risk to development partners. Clear requirements enable accurate estimation and budget certainty.
Hybrid models combining onshore management with offshore development optimize effectively. Organizations achieve 40% to 50% cost savings while maintaining quality standards. Communication practices and oversight processes determine success with distributed teams.
Build a Cost-Optimized EHR Without Compromising Quality
Our hybrid delivery model blends onshore healthcare architects with expert offshore teams to deliver compliant, high-performance EHR solutions within budget.
Ongoing EHR Development Costs
Initial development accounts for only a portion of total ownership expenses. Planning for ongoing costs prevents budget surprises and ensures system sustainability.
Annual maintenance costs
Budget 15% to 20% of the initial development cost annually for maintenance. This covers bug fixes, security patches, and minor feature updates. Maintenance costs remain relatively stable year over year.
Typical maintenance includes:
- Bug identification and resolution.
- Security vulnerability patching.
- Operating system and framework updates.
- Minor feature enhancements and improvements.
- Performance monitoring and optimization.
- Technical support for users.
- Documentation updates.
Infrastructure and hosting costs
Cloud hosting expenses vary based on user volume and data storage requirements. Small implementations may cost $500 to $2,000 monthly. Enterprise systems with high-availability requirements cost $10,000 to $25,000 per month.
Infrastructure cost factors include:
- Compute resources for application servers.
- Database storage and performance tiers.
- Content delivery and caching services.
- Backup and disaster recovery systems.
- Network bandwidth and data transfer.
- Security services and monitoring tools.
- Development and staging environments.
Compliance and security maintenance
Annual security audits and compliance activities require dedicated investment. Organizations should budget $20,000 to $50,000 annually for compliance maintenance. Regulated industries may face higher requirements.
Ongoing compliance activities include:
- Annual penetration testing and vulnerability assessments.
- Security audit preparation and documentation.
- Compliance certification renewals.
- Policy and procedure updates.
- Staff security training programs.
- Incident response planning and testing.
Enhancement and evolution costs
EHR systems require continuous improvement to maintain competitive positioning. Budget $50,000 to $200,000 annually for new feature development. Enhancement investments keep systems relevant as healthcare evolves.
Common enhancement areas include:
- New regulatory requirement implementations.
- Additional integration development.
- User experience improvements.
- Performance optimization initiatives.
- Mobile capability expansions.
- Analytics and reporting enhancements.
Factors That Increase EHR Development Cost
Certain project characteristics significantly push costs into higher ranges. Recognizing these factors helps set realistic budget expectations.
1. Legacy system integration complexity
Connecting to older systems without modern APIs creates substantial development work. Legacy platforms often lack documentation, requiring reverse engineering. Custom middleware development bridges connectivity gaps at a high cost.
Budget an additional $30,000 to $100,000 for each complex legacy integration. Allow extra time for discovery and troubleshooting. Consider phased approaches that address critical integrations first.
2. Multi-specialty clinical requirements
Different medical specialties have unique documentation and workflow needs. Cardiology, oncology, and behavioral health each require specialized modules. Supporting multiple specialties multiplies content and workflow development.
Specialty modules add $20,000 to $80,000 each, depending on complexity. Template libraries and clinical content require ongoing maintenance. Consider phased specialty rollouts to manage scope effectively.
3. Advanced AI and analytics capabilities
Artificial intelligence features require specialized expertise and significant development effort. Machine learning models need training data and ongoing refinement. Predictive analytics demand robust data architecture foundations.
AI capabilities add $50,000 to $200,000+ to baseline development costs. Consider starting with rule-based decision support. Add machine learning capabilities after core systems prove stable.
4. Stringent compliance certifications
Achieving specific regulatory certifications extends timelines and increases costs. ONC certification for EHR systems requires extensive documentation and testing. International certifications, such as CE marking for the European market, add complexity.
Certification processes add 20% to 40% to baseline project costs. External auditors and consultants may be necessary. Build certification timelines into project planning from inception.
5. Geographic distribution requirements
Multi-location deployments add significant architectural complexity. Data sovereignty requirements may mandate regional data storage. Network connectivity and synchronization create ongoing challenges.
Distributed architectures add 25% to 50% to development costs. High availability requirements further increase complexity. Consider cloud native approaches that simplify geographic distribution.
Best Practices for Managing EHR Development Costs
Following proven practices helps organizations maximize value from their EHR investments. To achieve this, many organizations choose to hire EHR developers who bring specialized expertise. These guidelines represent accumulated wisdom from successful implementations.
1. Invest adequately in discovery
Thorough discovery prevents expensive rework during later phases. Rushing requirements analysis creates gaps that surface during development. Comprehensive documentation aligns stakeholder expectations effectively.
Interview users at every level, from front desk staff to clinical leadership. Each perspective reveals different pain points and workflow needs. Observe actual work rather than relying solely on described processes.
Expect discovery to consume 10% to 15% of the total project budget. This investment prevents much larger expenses from scope changes. Quality discovery deliverables guide all subsequent project decisions.
2. Prioritize MVP features ruthlessly
Building everything at once increases cost and delays time to value when you develop an EHR MVP. Identify core features that deliver immediate clinical benefit. Defer nice-to-have capabilities to subsequent development phases.
Minimum Viable Product approaches reduce initial investment requirements. Launching sooner generates user feedback for improvement prioritization. Early adoption builds organizational momentum for continued investment.
Work with clinical stakeholders to identify truly essential capabilities. Focus on daily workflows rather than occasional processes. Build foundations that efficiently support future feature additions.
3. Select appropriate technology architecture
Technology choices impact both initial costs and long-term sustainability. Modern frameworks reduce development time by providing reusable components. Cloud native architectures simplify scaling and reduce infrastructure complexity.
Avoid bleeding-edge technologies without proven healthcare implementations. Established frameworks have larger talent pools and better documentation. Balance innovation with pragmatic risk management.
Consider the total cost of ownership when evaluating technology options. Open-source solutions eliminate licensing fees but require investment in support. Commercial platforms provide support but create vendor dependency.
4. Establish clear governance and communication
Project governance prevents scope creep and maintains budget discipline. Defined decision-making processes resolve conflicts quickly. Regular communication keeps stakeholders informed and engaged.
Weekly status reporting tracks progress against milestones and budget. Steering committees address escalated issues promptly. Clear escalation paths prevent small problems from becoming major obstacles.
Document all decisions and their rationale comprehensively. Written records prevent wasteful revisiting of settled questions. Governance documentation supports future enhancement planning.
5. Plan for iterative delivery
Delivering functionality incrementally provides visibility and reduces risk. Stakeholders see progress regularly and provide timely feedback. Course corrections happen before significant investment accumulates.
Two-week sprint cycles work well for most EHR development projects. Longer iterations delay feedback unnecessarily. Shorter cycles create coordination overhead without proportional benefit.
Prioritize delivery of core clinical workflows first. Users begin benefiting while additional features are being developed. Early value delivery builds organizational support for continued investment.
6. Build testing into the development process
Quality assurance investments prevent expensive post-launch remediation. Automated testing enables frequent validation of code changes. Security testing identifies vulnerabilities before they are exposed in production.
Budget 15% to 20% of development costs for comprehensive testing. Automated test suites provide ongoing regression protection. Manual testing validates user experience and workflow scenarios.
Include performance testing with realistic data volumes. Systems that work in development may struggle with production loads. Early performance validation prevents embarrassing launch failures.
7. Budget for ongoing evolution
EHR systems require continuous improvement to maintain value. Technology and regulations evolve constantly, requiring updates. User feedback reveals improvement opportunities continuously.
Budget 15% to 20% of the initial development cost annually for maintenance. Enhancement funding enables competitive positioning over time. Systems without investment stagnate and eventually require replacement.
Plan enhancement roadmaps based on user feedback and strategic priorities. Regular releases maintain user engagement and satisfaction. Continuous improvement demonstrates organizational commitment to clinical excellence.
Get a Detailed Cost Analysis for Your EHR Development Project
Space-O Technologies provides transparent pricing models and customized estimates aligned with your system complexity and compliance needs.
EHR Development Cost Comparison: Custom vs Commercial Solutions
Organizations must evaluate whether custom development or commercial licensing better serves their needs. Each approach has distinct cost characteristics and trade-offs.
Custom EHR development costs
| Cost Category | Investment | Ongoing Annual |
|---|---|---|
| Development | $50,000 to $1,500,000+ | N/A |
| Maintenance | N/A | 15% to 20% of development |
| Hosting | Included or separate | $6,000 to $120,000 |
| Enhancements | N/A | $50,000 to $200,000 |
| Compliance | Included | $20,000 to $50,000 |
Total 5 year cost for mid-sized implementation: $400,000 to $900,000
Commercial EHR licensing costs
| Cost Category | Initial Investment | Ongoing Annual |
|---|---|---|
| Licensing | $10,000 to $100,000 | $5,000 to $50,000 per provider |
| Implementation | $50,000 to $300,000 | N/A |
| Customization | $20,000 to $150,000 | $10,000 to $50,000 |
| Integration | $15,000 to $100,000 | $5,000 to $20,000 |
| Training | $5,000 to $30,000 | $2,000 to $10,000 |
Total 5 year cost for mid-sized implementation: $350,000 to $800,000
When custom development makes financial sense
Custom EHR development offers greater value in certain circumstances. Organizations with unique workflows that commercial systems cannot accommodate benefit significantly. Large user populations escape per-seat licensing fees that compound annually.
Companies seeking competitive differentiation through proprietary capabilities should consider custom solutions. Control over development roadmaps enables strategic technology investments. Independence from vendor business decisions protects long-term interests.
Healthcare technology startups building products for market sale need custom platforms. Commercial licenses typically prohibit resale or redistribution. Custom development creates intellectual property assets with business value.
When commercial solutions prove more cost-effective
Commercial EHR systems suit organizations with standard workflows and immediate needs. Proven implementations reduce deployment risk substantially. Existing customer bases provide validation and reference experiences.
Limited IT resources favor commercial solutions with vendor support. Managed services reduce internal staffing requirements. Organizations without development expertise benefit from turnkey approaches.
Tight timelines may preclude the use of custom development schedules. Commercial systems deploy faster when standard configurations suffice. Time-to-value matters when competitive or regulatory pressures are present.
Partner with Space-O Technologies for Your Custom EHR Development
Understanding the cost of EHR development is the first step toward building a secure and scalable healthcare solution. However, the success of your project depends not just on budgeting but on choosing the right development partner. A well-planned EHR system must balance functionality, compliance, interoperability, security, and long-term scalability without exceeding financial limits.
Reducing development costs does not mean compromising on quality or compliance. With the right architecture decisions, phased development strategy, and clear feature prioritization, healthcare organizations can build a HIPAA-compliant EHR system that delivers strong operational and financial returns.
With 15+ years of healthcare software development experience and 1200+ clients served, Space-O Technologies specializes in building secure, scalable, and cost-efficient EHR systems. Our team understands regulatory requirements, interoperability standards, cloud infrastructure planning, and budget optimization strategies that help healthcare providers maximize ROI.
If you are planning to develop a custom EHR system and want a transparent cost estimate tailored to your requirements, consult our healthcare software experts today. Let us help you build a compliant, future-ready EHR solution within your budget.
Frequently Asked Questions on EHR Development Cost
1. What is the average cost to develop an EHR system?
EHR development costs range from $50,000 for basic systems to $1,500,000 or more for enterprise implementations. Basic patient record management typically costs $50,000 to $120,000. Standard systems with comprehensive features range from $120,000 to $300,000. Advanced platforms with AI capabilities cost $300,000 to $600,000. Enterprise solutions for large health systems significantly exceed $600,000 significantly.
2. What factors most significantly affect EHR development cost?
Feature complexity, compliance requirements, and integration needs have the largest cost impact. The number and sophistication of clinical modules determine baseline scope. HIPAA compliance and security implementations add 15% to 30% to costs. Each external system integration adds $15,000 to $60,000, depending on complexity. The development team’s location and engagement model also substantially influence pricing.
3. How long does custom EHR development take?
Development timelines range from 3 months to 20 months, depending on the scope. Basic EHR systems typically require 3 to 5 months. Standard implementations take five to nine months. Advanced platforms require 9 to 14 months. Enterprise deployments last 12 to 20 months, including phased rollouts.
4. What are the ongoing costs after EHR development?
Plan for annual expenses equal to 20% to 30% of the initial development investment. Maintenance costs 15% to 20% of development annually for bug fixes and patches. Cloud hosting costs range from $6,000 to $120,000 per year, depending on scale. Compliance activities require $20,000 to $50,000 annually. Enhancement budgets of $50,000 to $200,000 keep systems competitive.
5. Is custom EHR development cheaper than commercial solutions?
Custom development may cost less over time for organizations with large user populations. Per-seat commercial licensing fees compound annually for five or more years. Organizations with 50 or more users often achieve lower total ownership costs. However, initial development requires a larger upfront investment than commercial implementation fees.
6. What is the minimum budget for an EHR MVP?
Minimum viable EHR products can launch with budgets starting around $50,000 to $80,000. This investment covers core patient management and clinical documentation. MVP approaches prioritize essential features to validate market fit quickly. Organizations should budget additional funding for post-launch iteration based on user feedback.
7. How can organizations reduce EHR development costs?
Several strategies effectively reduce EHR development costs. Prioritizing MVP features reduces initial scope and investment requirements. Offshore or hybrid development models offer significantly lower hourly rates. Phased delivery spreads investment over time while generating early value. Thorough discovery prevents expensive scope changes during development.
8. What hidden costs should we anticipate in EHR development?
Several cost categories often surprise organizations during EHR development. Legacy system integrations frequently exceed initial estimates by a substantial margin. Data migration complexity requires additional development effort. User training investments directly impact adoption rates. Ongoing compliance maintenance requires annual budget allocation. Infrastructure costs scale with user adoption and data volumes.



