Contents
The terms EHR and EMR are often used interchangeably in healthcare technology discussions, but they are not the same. While both systems digitize patient records, their scope, functionality, and interoperability capabilities differ significantly. Understanding these differences is critical when selecting the right healthcare software solution.
An electronic medical record system is typically designed to manage patient records within a single healthcare practice. An electronic health record system, on the other hand, is built to share patient information across multiple providers and healthcare organizations. This difference impacts everything from data accessibility and care coordination to scalability and compliance.
In this guide, we break down the key differences between EHR and EMR software. Based on our 15+ years of experience as a trusted healthcare software development agency, we have shared insights on the features, interoperability, benefits, and use cases of each to help you determine which solution best fits your healthcare organization’s needs.
What is an EMR (Electronic Medical Record)?
An EMR (Electronic Medical Record) is a digital version of the traditional paper chart used within a single healthcare practice. It stores patient diagnoses, treatment notes, medications, and test results in one centralized electronic system. Clinicians use it to track and manage medical data over time without manually searching through physical folders.
Think of an EMR as a digital notebook for a single doctor’s office. It holds valuable clinical information but stays confined to that one location. Other providers cannot access or update the records from external facilities, which creates challenges when patients visit specialists or receive emergency care elsewhere.
Key characteristics of EMR software
EMR systems are built to serve the internal documentation needs of a single healthcare organization. They replaced physical filing cabinets in clinics across the country, improving documentation accuracy and making record retrieval significantly faster for clinical staff.
Here are the defining characteristics of EMR software:
- Used within a single healthcare organization: EMR data typically stays locked within one practice or facility. It is not designed for cross-facility access or real-time collaboration between multiple providers.
- Digital version of paper charts: EMRs capture visit notes, prescriptions, immunization records, and lab orders electronically, eliminating the need for manual paper-based documentation.
- Limited interoperability: Sharing data with external providers often requires manual effort, such as faxing or printing. This closed design works well for isolated practices but limits broader care coordination.
- Provider-focused data management: The system is primarily designed for clinicians to document, review, and manage patient information internally rather than enabling patient-facing access or multi-provider collaboration.
Common EMR use cases
EMR systems are best suited for healthcare settings where clinical operations remain largely self-contained. The most common use cases include:
- Small clinics: Independent practices with a limited number of physicians use EMRs to digitize patient records and streamline day-to-day clinical documentation.
- Single-specialty practices: Specialty offices such as dermatology, orthopedics, or cardiology clinics rely on EMRs to manage condition-specific patient data within their own facility.
- Internal record digitization: Practices transitioning from paper-based workflows adopt EMR systems as the first meaningful step toward healthcare digitization, improving retrieval speed and documentation accuracy.
While EMRs serve their purpose well within a single practice, their limitations in data sharing and interoperability led to the development of a more connected solution — the EHR system.
What is an EHR (Electronic Health Record)?
An EHR (Electronic Health Record) is a comprehensive digital record designed to share patient data across multiple healthcare providers and facilities. Unlike an EMR, it goes beyond a single clinic and connects hospitals, specialists, labs, and pharmacies into one unified system. The record follows the patient across different care settings and geographic locations, allowing clinicians at separate facilities to access the same updated medical information seamlessly.
EHR platforms support interoperability through recognized standards like HL7 and FHIR. These protocols allow different software applications to exchange clinical data securely. The 21st Century Cures Act requires certified platforms to offer FHIR-based APIs, which continues to drive widespread adoption of connected health record solutions nationwide.
Key characteristics of EHR software
EHR systems are built to support coordinated, patient-centered care across the entire healthcare ecosystem. They go far beyond internal documentation by enabling real-time data exchange, patient engagement, and advanced clinical insights.
Here are the defining characteristics of EHR software:
- Cross-provider data sharing: EHR platforms allow hospitals, specialists, labs, and pharmacies to access and update the same patient record. Clinicians at separate facilities view real-time medical information without relying on faxes or manual transfers.
- Interoperability capabilities: EHR systems use standardized protocols like HL7 and FHIR to exchange clinical data securely between different software applications. This ensures seamless communication across diverse healthcare technologies.
- Patient-centered records: Unlike EMR tools, electronic health records include patient portals and mobile access features. Patients view their records, download documents, and message their care teams directly, making them active participants in their own care.
- Longitudinal health data: EHR systems capture a patient’s complete medical history across every provider, visit, and care setting over time. This comprehensive view enables more informed clinical decisions and supports long-term health tracking.
Common EHR use cases
EHR systems are best suited for healthcare organizations that operate across multiple locations or coordinate care with external providers. The most common use cases include:
- Hospitals: Large hospital systems rely on EHR platforms to manage complex patient workflows, coordinate between departments, and maintain compliance with federal interoperability mandates.
- Multi-location healthcare groups: Organizations operating clinics across different cities or regions use EHR systems to unify patient records and ensure consistent care delivery regardless of location.
- Integrated care networks: Networks that bring together primary care physicians, specialists, labs, and pharmacies adopt EHR platforms to enable real-time data sharing, population health management, and clinical decision support across the entire care continuum.
EHR systems also provide advanced analytics and clinical decision support, helping care teams identify disease trends and improve treatment outcomes at scale. Organizations that adopt EHR platforms position themselves for long-term regulatory compliance, operational efficiency, and growth.
Key EHR vs EMR Differences You Should Understand
Understanding the core distinctions helps providers select the right platform for their operations. Many clinics invest in EMR solutions without realizing they actually need EHR capabilities.
The differences affect data sharing, compliance, patient engagement, and organizational growth. Below is a detailed comparison that clearly highlights all important distinctions.
| Aspect | EMR (Electronic Medical Record) | EHR (Electronic Health Record) |
|---|---|---|
| Scope | Single practice or provider only | Across multiple providers and organizations |
| Data Sharing | Limited to one facility | Designed for interoperability across systems |
| Data Portability | Records stay within one location | Records follow the patient across care settings |
| Use Cases | Diagnosis and treatment within one clinic | Care coordination, population health, and research |
| Regulatory Compliance | Basic HIPAA compliance | HIPAA plus Meaningful Use plus FHIR mandates |
| System Integration | Minimal lab and billing connections | Full integration with labs, pharmacies, imaging, and payers |
| Patient Access | Limited or no patient interaction | Patient portals, mobile apps, and FHIR APIs |
| Analytics | Basic internal reporting only | Population health analytics and clinical decision support |
| Best Suited For | Solo practices and small clinics | Hospitals, health systems, and multi-provider networks |
The comparison reveals fundamental differences in scope, connectivity, and clinical value. EMR platforms serve narrow documentation needs within a single practice environment. EHR systems provide broader functionality to support modern healthcare delivery requirements. Choosing the wrong platform creates costly obstacles as your organization expands its services.
Detailed Differences Between EHR and EMR
The comparison table above highlights the core distinctions between EHR and EMR systems at a glance. However, each difference carries practical implications that directly affect how healthcare organizations manage patient data, meet regulatory requirements, and scale their operations. This section evaluates both systems across every key aspect to help you make a more informed decision.
1. Scope
EMR systems operate within the boundaries of a single practice or provider. All clinical data stays confined to one organization, making it suitable for independent offices that manage care entirely in-house.
EHR systems extend across multiple providers, facilities, and organizations. They are built to support coordinated care delivery across hospitals, specialty clinics, labs, and pharmacies simultaneously.
2. Data sharing
EMR platforms limit data sharing to one facility. Transferring records to an external provider typically requires manual processes like faxing or printing, which slows down care coordination.
EHR systems are designed for interoperability from the ground up. They use standardized protocols like HL7 and FHIR to exchange clinical data securely across different healthcare systems in real time.
3. Data portability
With an EMR, patient records remain locked within one location. If a patient visits a new provider, their medical history does not follow them automatically.
EHR systems enable records to travel with the patient across different care settings. Whether a patient visits a specialist, an urgent care center, or a hospital in another city, their complete medical history remains accessible.
4. Use cases
EMR systems are built for straightforward clinical documentation, primarily supporting diagnosis and treatment workflows within a single clinic.
EHR systems serve a much broader range of functions, including care coordination between multiple providers, population health management, and clinical research across the entire care continuum.
5. Regulatory compliance
EMR platforms typically meet basic HIPAA compliance requirements for data privacy and security within a single practice.
EHR systems must satisfy more rigorous regulatory standards, including HIPAA, Meaningful Use criteria, and FHIR-based interoperability mandates under the 21st Century Cures Act.
6. System integration
EMR tools offer minimal integration, usually limited to basic lab and billing connections within the practice.
EHR platforms provide full integration with external systems, including laboratories, pharmacies, imaging centers, and insurance payers, eliminating manual data entry and reducing errors across the care network.
7. Patient access
EMR systems offer limited or no direct patient interaction. Patients typically cannot view their records or communicate with their care team through the platform.
EHR systems include patient portals, mobile applications, and FHIR APIs that give patients direct access to their health information, including test results, prescription refills, and provider messaging.
8. Analytics
EMR platforms support basic internal reporting, such as tracking visit volumes or generating simple clinical summaries within the practice.
EHR systems provide advanced analytics capabilities, including population health tracking, clinical decision support, and predictive modeling to improve patient care at scale.
9. Best Suited For
EMR systems work best for solo practices and small clinics that manage care independently without frequent external referrals.
EHR systems are better suited for hospitals, health systems, and multi-provider networks that require seamless data exchange, regulatory compliance, and coordinated care delivery across multiple locations.
Understanding these differences is critical because choosing the wrong platform creates costly obstacles as your organization expands its services. The next step is evaluating which system aligns with your specific operational needs, growth plans, and compliance requirements.
Not Sure Whether You Need an EMR or EHR?
Get a free assessment from Space-O Technologies. Our healthcare technology experts help you evaluate your requirements and recommend the right platform for your clinical goals.

When Should You Choose an EMR?

EMR systems remain a practical choice for specific practice types and operational scenarios. Not every healthcare facility needs the full scope of an EHR platform immediately. Certain conditions make EMR tools the right fit for your current stage of growth. Consider adopting an EMR platform in the following situations.
- Solo practice with no referral network. You operate independently without regular data exchange with outside providers or specialists.
- Limited budget for technology investment. Your practice needs digital documentation, but cannot fund a comprehensive EHR deployment at this time.
- Simple clinical workflows. Your daily operations involve straightforward patient visits that do not require multi-system connectivity or external coordination.
- No immediate regulatory pressure. Your practice type or size does not yet face federal mandates requiring certified EHR technology or interoperability compliance.
- Paper-to-digital transition. You are moving from paper charts to electronic records for the first time and want a simpler starting point initially.
Even in these scenarios, providers should plan for future EHR migration as their needs evolve. Regulatory requirements continue expanding, and patient expectations for digital access keep increasing. Starting with an EMR today does not mean staying with it permanently. A forward-looking technology strategy helps avoid costly emergency transitions down the road.
When Should You Choose an EHR?

EHR platforms deliver the best value for practices that need connectivity, compliance, and scalability. Most modern healthcare facilities benefit from full EHR adoption regardless of their current size. The following scenarios strongly indicate that an EHR system is the right investment. Evaluate your operations against these criteria before making a final decision.
- Multi-provider or multi-location practice. You operate across several sites and need staff to access patient records from any facility within your network.
- Active referral and specialist coordination. Your patients regularly see external specialists who need access to updated clinical information promptly.
- Federal compliance requirements. Your organization must meet Meaningful Use, MIPS, or the 21st Century Cures Act mandates for certified health record technology.
- Patient portal demand. Your patients expect digital access to records, test results, appointment scheduling, and secure messaging features today.
- Population health and analytics goals. You want to track clinical outcomes, identify risk patterns, and actively participate in value-based care programs.
- Growth and expansion plans. You plan to add locations, departments, or service lines that require a scalable, interconnected technology foundation soon.
Providers who meet even two of these criteria should strongly prioritize EHR adoption. The platform pays for itself through improved efficiency, fewer errors, and regulatory compliance. Delaying the transition only increases future migration costs and compliance risks. Investing in EHR technology today prepares your organization for the next decade of healthcare delivery.
Let Our Experts Manage Your RPM Modernization Journey
Discuss your clinical requirements with Space-O Technologies. We help healthcare organizations evaluate, select, and implement the right health record platform for lasting results.
How to Migrate from EMR to EHR Successfully
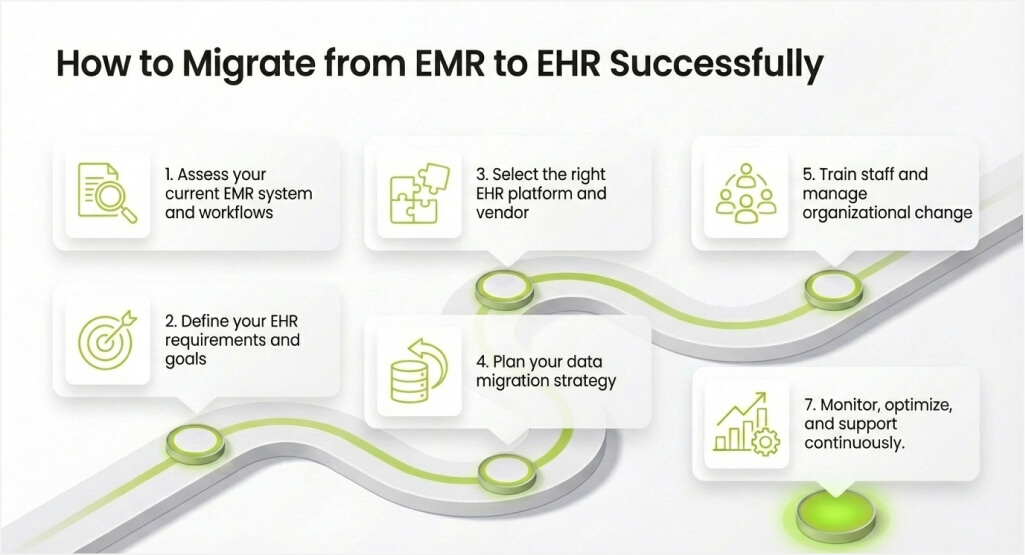
Transitioning from an EMR platform to a full EHR system requires careful planning and execution. Rushed migrations create data quality problems, workflow disruptions, and staff resistance. A structured approach protects your clinical operations while gradually unlocking new capabilities. Follow these steps to ensure a smooth and successful migration process.
Step 1: Assess your current EMR system and workflows
Document every feature your existing platform provides and how staff uses it daily. Identify gaps between your organization’s current capabilities and the functionality it actually needs. Map clinical workflows to understand how data moves through your practice today. This assessment reveals migration priorities and helps define requirements for the new EHR platform.
Step 2: Define your EHR requirements and goals
List the specific capabilities your new system must deliver for your organization. Clearly include interoperability needs, patient portal features, analytics tools, and compliance requirements. Align technology goals with your broader business strategy and growth plans intentionally. Clear requirements prevent scope creep and keep the selection process focused on real priorities.
Step 3: Select the right EHR platform and vendor
Carefully evaluate potential platforms against your documented requirements and budget constraints. Request demonstrations, references, and details on integration capabilities directly from each vendor. Verify that the platform holds ONC certification and supports native FHIR-based data exchange. The right vendor becomes a long-term partner, not just a software supplier to your practice.
Step 4: Plan your data migration strategy
Determine which records, templates, and historical data must transfer to the new platform. Clean existing data by removing duplicates, correcting errors, and standardizing formats beforehand. Map data fields from your EMR to corresponding elements in the EHR system accurately. Test migration scripts thoroughly in a sandbox environment before touching production data.
Step 5: Train staff and manage organizational change
Develop role-based training programs that address each team member’s specific daily workflows. Schedule sessions before, during, and after the go-live date to reinforce learning continuously. Designate superusers in each department to provide peer support during the transition. Effective change management reduces resistance and accelerates adoption across your entire organization.
Step 6: Execute a phased deployment
Launch the new EHR in stages rather than switching everything at once across the practice. Start with one department or location and expand gradually based on lessons learned. Monitor performance, gather user feedback, and resolve issues before rolling out to additional areas. A phased approach minimizes disruption and steadily builds confidence among staff members.
Step 7: Monitor, optimize, and support continuously
Track system performance, user adoption rates, and data quality metrics after every deployment phase. Address issues quickly and adjust configurations based on real-world usage patterns observed. Establish ongoing support resources to help staff troubleshoot problems and request enhancements. Continuous improvement ensures your EHR investment delivers maximum value over its entire lifecycle.
A disciplined migration approach saves time, money, and frustration for everyone involved. Providers that skip steps often face rework that doubles their original project timeline estimate. Investing in proper planning builds a robust, lasting foundation for connected healthcare delivery.
Outgrowing Your Current EMR System?
Upgrade to a fully integrated EHR solution with Space-O Technologies. Our experts help you migrate seamlessly without disrupting daily clinical operations or patient care delivery.
Partner with Space-O Technologies for the Right Health Record Solution
The differences between EHR and EMR go far beyond simple terminology or feature lists. Choosing the right system affects patient outcomes, regulatory standing, operational efficiency, and long-term growth. Providers who understand these distinctions make technology decisions that strengthen their practice. Those who overlook them risk compliance gaps and care coordination failures.
Whether you need a focused EMR for a solo practice or a full-scale EHR for a health system, selecting one requires expert guidance. Building or customizing a health record platform requires deep knowledge of clinical workflows and technical expertise. Security, interoperability, and regulatory compliance must be part of the solution from day one. A thoughtful approach saves significant resources over the platform’s lifetime.
Space-O Technologies specializes in custom health record solutions for healthcare organizations of every size. Our experienced teams help you evaluate your needs, select the right platform, and build secure, compliant systems. From initial assessment through deployment and ongoing support, we deliver results that matter. Talk to our specialists and take the next step toward better healthcare technology today.
FAQs About EHR vs EMR Differences
1. What is the main difference between EHR and EMR?
The main difference lies in the scope of data sharing. An EMR stores patient records within a single practice and does not share data externally. An EHR connects multiple providers and enables clinical information exchange across hospitals, specialists, and pharmacies. EHR platforms follow the patient across care settings while EMR records stay in one location.
2. Can a small practice use an EHR instead of an EMR?
Yes, small practices can adopt EHR systems and benefit from interoperability and patient engagement features. Cloud-based EHR platforms offer affordable subscription models designed specifically for smaller organizations. The investment pays off through improved compliance, better care coordination, and enhanced patient satisfaction. Many vendors offer scaled-down EHR solutions that suit independent practices perfectly.
3. Is it mandatory to use an EHR in the United States?
Federal programs such as Meaningful Use and MIPS incentivize eligible providers to adopt certified EHRs. The 21st Century Cures Act mandates interoperability and FHIR-based API access for certified platforms. While no single law requires every practice to adopt an EHR, non-participation carries financial penalties. Most providers find that compliance requirements effectively make EHR adoption necessary today.
4. How much does it cost to migrate from EMR to EHR?
Migration costs depend on your current system, data volume, and the EHR platform you select. Small practices typically invest between $20,000 and $75,000 for a complete transition. Larger organizations with complex data and multiple locations may spend $150,000 or more. Working with experienced partners helps control costs and avoid unexpected budget overruns during migration.
5. What does PHR mean, and how is it different from EHR and EMR?
A Personal Health Record (PHR) is a health data platform managed entirely by the patient. Unlike EMR and EHR systems controlled by healthcare providers, PHR tools let individuals track their own records. Patients independently store medication lists, allergy information, fitness data, and vaccination histories. Many PHR apps now sync with EHR platforms through FHIR APIs for seamless data sharing.
6. Which is better for a hospital, EHR or EMR?
Hospitals benefit significantly from EHR systems due to their interoperability and data-sharing capabilities. An EMR cannot support the multi-department coordination required in hospital operations. EHR platforms connect emergency departments, surgical units, laboratories, and pharmacy systems together seamlessly. For any facility with multiple care teams, an EHR is the clear and recommended choice.



